Top 10 Myths About the Contraceptive Pill

When it comes to the subject of contraceptive pills, haven’t most of us heard whispers like “pills cause infertility” or “only married women should use them”? Myths like these stir anxiety, fuel stigma, and often delay informed decisions – and that just isn’t fair. From random WhatsApp forwards to well-meaning but misinformed advice, it’s tough to separate fact from fear. Many women silently navigate confusion, side-eye judgement, and endless what-ifs around a pill meant to help. At Eva Woman Care Clinic, we hear these concerns daily – and we’re here to clarify, support, and guide you with zero judgement. Whether you’re managing PCOS or just want clarity, our expert doctor Dr Grishma Ranjangaonkar offers the answers you deserve. Myth 1: Contraceptive pills cause significant weight gain “You’ll gain loads of weight if you start the pill.” Sound familiar? This is one of the most common myths we hear. The truth is, any weight changes are usually small and temporary. Some women may retain water due to hormonal shifts, but it typically stabilises within a few months. Activity levels, eating habits, and family history play a much larger role in long-term weight trends than the pill itself. Our team frequently helps women understand how to manage side effects with simple lifestyle tweaks. Myth 2: Birth control pills lead to infertility Worried that taking the pill will stop you from getting pregnant later? It won’t. Most women regain their fertility within a month or two of stopping the pill. Even women using it for years conceive easily when they choose to. The confusion often stems from injectable methods like Depo-Provera, which can take several months longer for fertility to return. At Eva Woman Care, we explain how different options work so you’re not left second-guessing your future plans. If you have any questions about infertility or birth control options, we welcome you to visit us for a thoughtful and informative chat. Myth 3: All contraceptive pills must be taken at the same time every day Telling all women to take their pills at the “exact same time or else” is misguided. It depends on the pill type. Combination pills offer a bit of flexible timing; a few hours’ delay won’t change effectiveness much. But with progestin-only pills – also called mini-pills – timing matters more. A delay of over three hours can reduce protection. Using phone alarms or scheduling it around daily routines can help build consistency with ease. Myth 4: Breastfeeding is a reliable contraceptive method Yes, breastfeeding affects fertility – but only under strict conditions. The method called LAM (Lactational Amenorrhea Method) works for up to six months only if you’re exclusively breastfeeding and haven’t had periods. A missed feed or the return of menstruation reduces its reliability. At our clinic, we recommend back-up birth control like the mini-pill or IUD for postpartum women who want to avoid surprises while breastfeeding. Myth 5: You need to take a break from using pills periodically The idea that the body needs a “rest” from birth control is outdated. In fact, breaks can lead to unwanted pregnancy. The pill was designed for long-term use and doesn’t lose effectiveness over time. Some injectable options may affect bone density, but pills don’t carry this concern. Regular check-ups, like the ones we offer at our clinic, help monitor overall wellness and adjust methods if needed – not because the body “gets used” to it. Myth 6: Emergency contraception is the same as abortion This belief not only spreads fear – it’s plain wrong. Emergency contraception prevents ovulation; it doesn’t end a pregnancy. If fertilisation has already occurred, emergency pills won’t have an effect. Unlike abortion pills, they don’t harm a developing embryo or interfere with implantation. We often meet women feeling guilty for using it, but there’s no need for shame. It’s a safe and legal backup option when things don’t go as planned. Myth 7: Newer brands of pills are more risky than older ones New doesn’t mean unsafe. Updated pills often contain lower hormone doses and are crafted to reduce side effects like nausea or acne. The risk of blood clots exists, but it’s rare and higher in women with certain medical conditions. That’s why we take medical history so seriously during contraceptive counselling. At Eva Woman Care Clinic, we personalise your pill choice to your health profile – not just what’s “old” or “new.” Myth 8: Contraceptive pills negatively affect libido and mood for everyone Some women notice mood shifts or changes in desire, but these effects vary wildly between individuals. Just like moods fluctuate naturally, hormonal combinations can influence each body differently. Feeling low or losing interest in intimacy isn’t an automatic pill effect. Often, a brand switch or taking a different formulation can resolve the issue. With our guidance, patients find solutions that balance physical and emotional well-being. Myth 9: The pill protects against sexually transmitted diseases The pill does quite a bit – but it can’t fight infections. It prevents pregnancy, not STDs. Condoms, both male and female, provide that barrier protection. That’s why we always promote dual protection, especially for those with new or multiple partners. Combining a condom with a reliable pill offers both pregnancy prevention and STD defence. It’s smart and safer. Myth 10: Only women are responsible for contraception Contraception isn’t a one-woman job. While many methods are geared toward females, men play a crucial role too. Condoms and vasectomy are valid options and should be part of the conversation. At our clinic, we encourage couples – married or not – to make birth control a shared topic. When both partners contribute, it becomes less stressful and more supportive. Additional Insights on Health and Safety Non-contraceptive health benefits of oral pills Beyond pregnancy prevention, oral pills help manage issues like acne, polycystic ovaries, and painful periods. Women with irregular bleeding often find relief as the pill regularises their cycles. Some rely on it to reduce heavy flow or ease intense cramps. At
Benefits of Laparoscopic Surgery Over Open Surgery
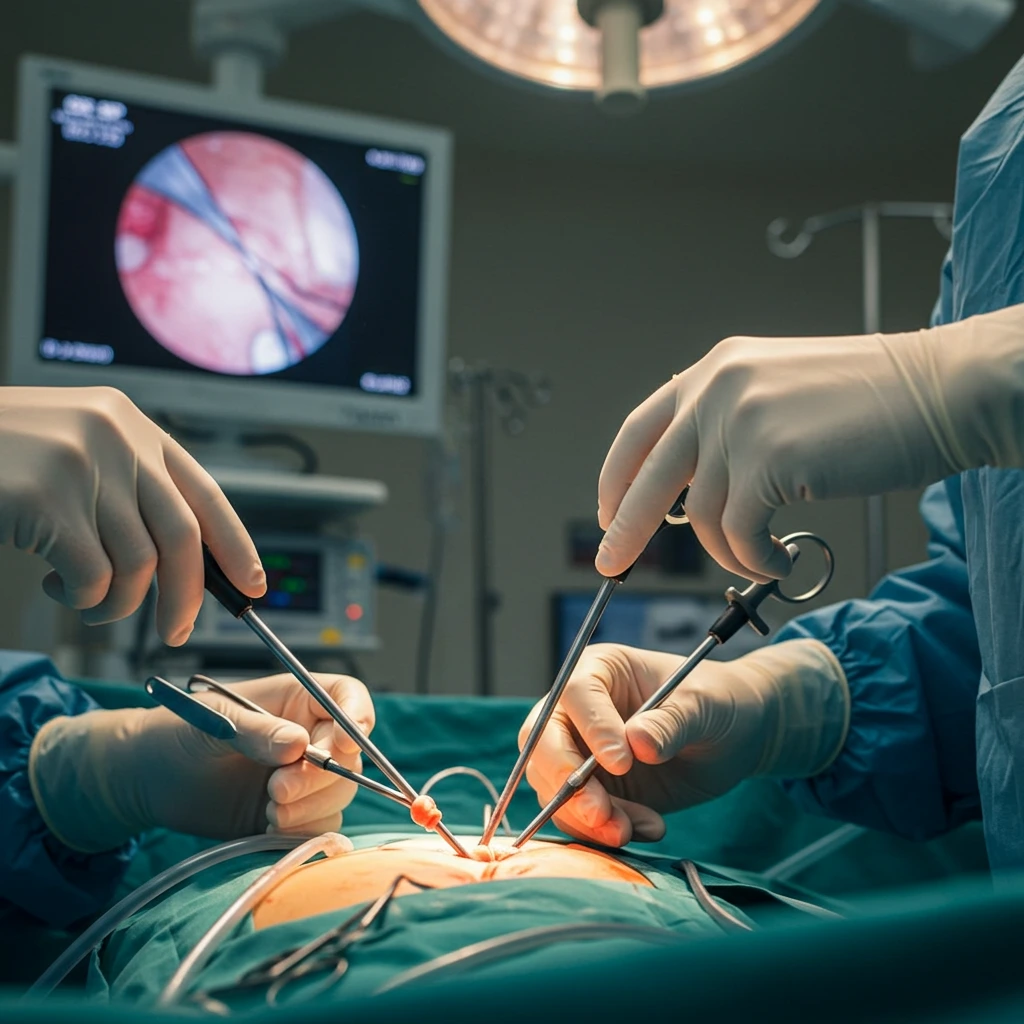
Going under the knife is never easy, especially when recovery feels like climbing a mountain in slippers. For women juggling work, home, or planning a family, long hospital stays and painful wounds can be exhausting. That’s why many are turning to laparoscopic surgery – less pain, fewer scars, and quicker bounce-back time. But yes, there’s still confusion around safety, cost, and the right time to consider it over open surgery. At Eva Woman Care Clinic, we guide you through every decision – from diagnosis to choosing what’s safest and most effective for you. Whether it’s fibroids, endometriosis, or fertility procedures, we make sure you heal with confidence and care. What is Laparoscopic Surgery? Laparoscopic surgery feels like a smoother road compared to traditional cuts and stitches. This minimally invasive method uses a tiny camera, called a laparoscope, and ultra-thin tools through a few small incisions. We rely on this approach daily at Eva Woman Care Clinic to treat fibroids, cysts, infertility conditions and more. It allows speedy access to organs with less disruption to surrounding tissue. The high-definition view helps guide every surgical move with near-perfect accuracy. From clearer vision to less internal trauma, this approach pairs safety with smart innovation that today’s women deserve. What is Open Surgery? Open surgery is the traditional format many are familiar with – it involves making a long incision for direct access. While it’s effective, especially in emergencies or complex cases, it tends to demand a longer healing period and greater care post-op. We still consider open surgery in situations where visibility needs to be broad, or instruments can’t reach deeply enough laparoscopically. However, with it comes higher risks like infections, scarring, and post-operative pain, which can sometimes set back recovery and independence. Comparison Between the Two Approaches One look at scars can tell the difference between these approaches. Laparoscopic surgery leaves tiny marks, while open surgery may leave a larger, more visible one. In the case of laparoscopy, fewer incisions also mean less blood loss and shorter anaesthesia exposure. Laparoscopy gives better visual access through high-resolution monitors and allows delicate movements in hard-to-reach areas. Open surgery provides a wider field but often causes more physical disruption, leading to longer recovery and increased discomfort for the patient. Clinical and Recovery Benefits of Laparoscopic Surgery Every woman wants to bounce back to her everyday life as soon as possible. That’s the beauty of laparoscopy. Healing is faster, scars are smaller, and discomfort is reduced. At Eva Woman Care Clinic, we follow strict protocols that combine advanced science with thoughtful patient care – for recovery that’s measured in weeks, not months. Faster Healing and Shorter Recovery Period No one likes staying in hospitals longer than needed. With laparoscopy, many patients go home the same day or the next morning. The muscles aren’t cut deeply, so the body heals more naturally and gently. Light activities are possible within days, and most resume normal routines in about two to three weeks. Our care plans at Eva include follow-up checks and clear instructions so women can heal confidently and comfortably from home, without the dragging pace often linked to open procedures. Reduced Post-operative Pain Gentler cuts mean gentler healing. That’s one reason most of our patients report significantly less pain after laparoscopic procedures. Since muscles and tissues aren’t pulled apart harshly, even pain medication is needed less often. That’s a blessing for those who want to avoid strong drugs or are planning pregnancy soon. Early mobility becomes possible, allowing women to walk, freshen up, and dine on their own soon after surgery. It’s these comforts that make a world of difference. Lower Risk of Complications and Infections Every small incision means a smaller chance of infection. Because there’s less exposure of internal organs and minimal cutting, the chances of internal bleeding or adhesions reduce dramatically. This cleaner, more targeted method makes post-operative headaches less likely. We at Eva Woman Care Clinic maintain sterile environments and advanced safety measures, which combine perfectly with laparoscopy’s clean, efficient nature to keep surgery outcomes predictable and reliable. Minimal Scarring and Aesthetic Outcome Post-surgery, looking in the mirror should feel reassuring, not upsetting. Laparoscopic surgery leaves behind just a few tiny marks on the skin – almost like faded dots over time. There’s less damage to surrounding tissues, reducing the chance of raised or irregular scars. Many of our patients feel emotionally lighter, knowing their bodies aren’t marked with large scars. This visual recovery plays a quieter, yet powerful, role in healing after surgery. Role in Specific Surgical Applications Laparoscopy isn’t just a concept; it’s a daily solution for women across different gynaecological conditions. From emergencies like appendicitis to planned procedures such as hysterectomy, the technique proves versatile. At Eva Woman Care, we apply laparoscopy across diagnostics, treatments and fertility-focused procedures, offering a comprehensive approach tailored for every unique case. Common Laparoscopic Procedures Our team performs several common surgeries using laparoscopy – each benefiting from smaller wounds and quicker recovery. Among the top are appendectomies, gallbladder removals, and colorectal treatments. By avoiding bulky incisions, we help ensure these surgeries don’t become long-term disruptions in your life. Colorectal surgeries, for example, require precision. Laparoscopy lets us handle these with accuracy, limiting the trauma while still offering effective results. Gynaecological and Urological Surgeries Whether it’s removing an ovarian cyst or restoring fertility steps, laparoscopy gently steps in. We use this approach for hysterectomies, fibroid removals, and tubal surgeries – especially where fertility preservation is a concern. For urological needs, like pelvic organ prolapse or endometriosis that affects the bladder, laparoscopy helps reduce surgical strain while offering excellent clinical outcomes. Precision is key, and our tools give just that level of control and safety. Bariatric and Abdominal Interventions Managing weight-related issues can require surgery. For those seeking relief from morbid obesity or digestive complications, laparoscopic options offer effective results with fewer risks. Compared to open bariatric procedures, these methods lower blood loss and limit tissue handling, contributing to safer outcomes. We also apply minimal incision
