Foods to Avoid During Pregnancy: A Simple Guide for Expecting Moms

Pregnancy is such a beautiful journey, but it also comes with many questions, especially when it comes to food. With so many suggestions from family, friends, neighbours, and even WhatsApp forwards, it can feel overwhelming to figure out what’s actually safe. At Eva WomanCare Clinic in Vashi, we believe that nourishing your body is one of the most loving things you can do for yourself and your baby. In this guide we are talking through the confusion to give you a clear, easy-to-follow list of foods to avoid during pregnancy. What Should I Avoid During Pregnancy? 1. Raw or Undercooked Eggs Foods like homemade mayonnaise, raw cookie dough, half-boiled eggs, and some desserts may contain uncooked eggs. These can carry bacteria like salmonella, which can cause severe stomach issues. You can however eat fully cooked eggs (bhurji, omelettes, hard-boiled), and bakery-made desserts with your doctor’s guidance. 2. Raw or Undercooked Meat and Seafood It is important to avoid dishes like rare steaks, sushi made with raw fish, undercooked chicken, or seafood that isn’t fully steamed or cooked. Raw meat often carries harmful bacteria that may lead to infections. Instead, you can choose well-cooked chicken, fish, prawns, mutton, eggs, and seafood dishes prepared thoroughly. 3. Unpasteurised Milk and Milk Products In India, raw milk or loose milk sold without proper processing is common. Avoid drinking unboiled milk or using products made from it, including unpasteurised paneer, raw milk or any homemade dairy products unless boiled You can opt for packaged milk (after boiling), pasteurised paneer, curd, and cheese. 4. Certain Types of Fish High in Mercury Did you know that although fish is a great source of protein, some varieties contain high mercury levels, which may harm your baby’s developing brain? After confirming with your doctor, you can safely eat fish like Pomfret, Surmai, Rawas, or Bangda (in moderation) Always ensure it’s cooked well. 5. Street Foods Prepared in Unhygienic Conditions Arent’ Mumbai street food absolutely tempting? Pani puri, vada pav, samosa, kebabs – but in pregnancy, hygiene matters more. Why to avoid it? Because there is a high risk of infection, contaminated water or unclean storage. Good news is that you can however eat home-made chaats, pani puri water, or pav bhaji at home using clean ingredients! 6. Soft Cheeses Made from Unpasteurised Milk Cheeses like Brie, Camemberti, and some imported soft cheeses can carry bacteria harmful during pregnancy. Check labels for “pasteurised.” Most Indian cheese varieties are safe. 7. Packaged or Processed Foods High in Preservatives Instant noodles, packaged chips, meat cold cuts, frozen sausages, and overly processed snacks offer little nutrition and may contain additives. You can opt for fresh home-cooked meals, roasted snacks, fruits, nuts, and balanced homemade recipes. 8. Raw Sprouts Raw sprouts like moong, alfalfa, or broccoli sprouts can sometimes carry bacteria because they grow in warm, moist conditions. To enjoy them safely during pregnancy, it’s best to have them lightly sautéed or boiled. 9. Excess Caffeine Did you know that enjoying a cup of chai or coffee is perfectly fine during pregnancy, but too much caffeine can affect your baby’s growth? A safe limit is about one to two cups of chai a day or one small coffee. It’s best to avoid energy drinks and very strong coffees. This guidance also assumes your sugar intake is kept within healthy limits. 10. Herbal Teas and Remedies Without Doctor Approval Many herbal teas like strong hibiscus, liquorice, or slimming teas may trigger contractions or affect hormone levels. Always check with your gynaecologist before using any herbal product. 11. Alcohol and Smoking These are unsafe at any stage of pregnancy. Even small amounts can affect the baby’s development. 12. Excess Papaya and Pineapple (Especially Raw) Raw or semi-ripe papaya contains latex, which is traditionally avoided in early pregnancy. Large amounts of pineapple are also often avoided. Moderate amounts of ripe papaya are usually safe, but it is always best to check with your doctor first! What You Can Eat Instead Don’t worry, you still have plenty of delicious and nutritious options! ✔︎ Fresh fruits (mangoes, apples, chikoo, grapes, pomegranates) ✔︎ Dal, roti, rice, khichdi ✔︎ Home-cooked vegetables ✔︎ Paneer, tofu, eggs ✔︎ Well-cooked fish and chicken ✔︎ Hydrating drinks like coconut water, lemon water, chaas ✔︎ Nuts, seeds, dates, and homemade laddoos for energy Pregnancy doesn’t have to feel restrictive, it’s simply about making mindful choices that support you and your baby. At Eva WomanCare Clinic, we’re here to guide you with warmth, clarity, and care, so every decision feels lighter, reassuring, and truly right for you. When to Contact Your Doctor? If you experience severe vomiting, loose motions after eating something, lower abdominal pain, unusual fatigue or fever or chills, reach out to your doctor immediately. Get Expert Pregnancy Support At Eva WomanCare Clinic in Vashi, Navi Mumbai, we guide expecting mothers with personalised nutrition, safe pregnancy care, and compassionate support. Whether you’re confused about what to eat, what to avoid, or how to stay healthy, we’re here to make your journey smoother and safer. Have any more questions? Contact us today!
What is an NT Scan in Pregnancy?
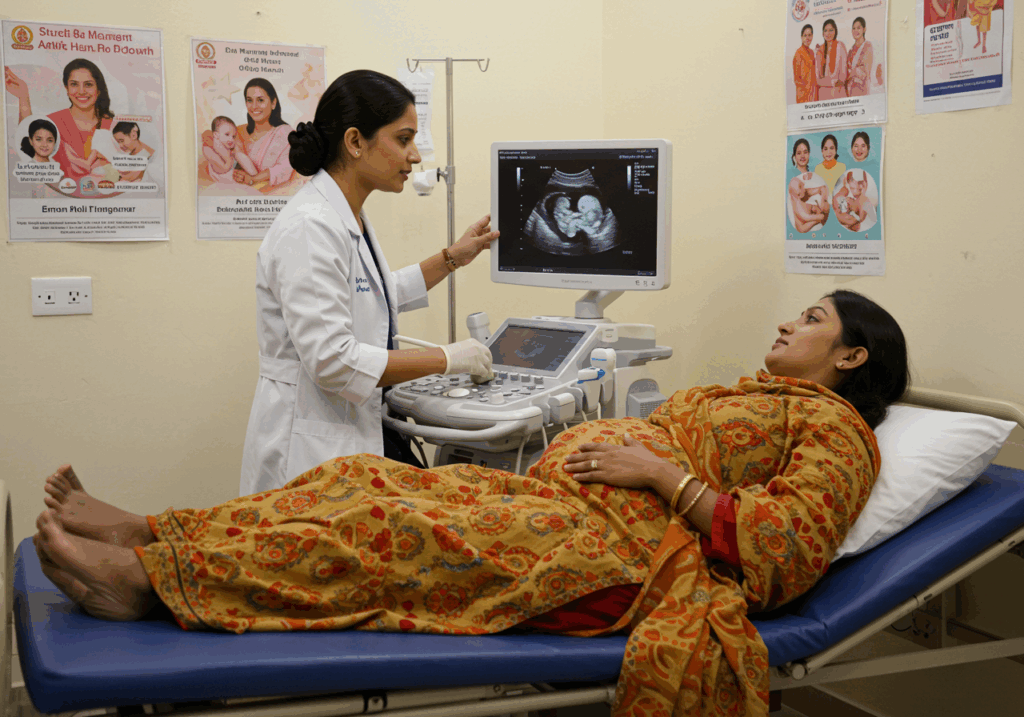
Watching a baby grow inside you feels magical, but the worry over health checks often quietly creeps in. If you’ve ever felt lost in a fog of test names and timing, you’re not alone-NT Scan often tops that list. It’s done early in pregnancy and feels like one more exam you don’t fully understand but have to face. Questions about safety, accuracy, or what it really shows can weigh heavier the more you read online. At Eva Womancare Clinic, we walk with you – answering every question, clearing the confusion, and offering real support. Whether you’re an expectant working woman or a first-time mom, we help you feel prepared and cared for. What is an NT Scan in Pregnancy? With 25+ years in women’s healthcare, Eva Womancare Clinic in Vashi provides trusted first-trimester expertise for expecting mothers. Among the earliest and most important tests is the NT scan-a non-invasive ultrasound that offers vital clues about your baby’s development. This test measures the clear space at the back of your baby’s neck and helps our team check for possible chromosomal conditions. We integrate NT scans into our comprehensive prenatal checkups to support healthy beginnings and confident parenthood. Definition and Importance NT scan stands for Nuchal Translucency Scan and is typically performed between 11 to 14 weeks of pregnancy. It helps evaluate risk of chromosomal abnormalities, including Down syndrome, by measuring fluid at the back of the baby’s neck. This scan also checks for nasal bone visibility and other early developmental signs. At Eva Womancare clinic, this is part of our early screening focus, offering expectant mothers clear insights into their baby’s wellbeing. When and Why It’s Done The best time for an NT scan is between the 11th and 13th week of pregnancy. It provides early indicators of genetic conditions and helps our doctors identify any additional investigations you may need. We recommend this scan for all pregnant women, especially those 35 and older or with a history of genetic concerns. Since it’s done only once during the first trimester, scheduling at the right moment is important for effective results. Understanding How NT Scan Works The NT scan may feel like a regular ultrasound, but beneath it lies advanced science that studies markers invisible to the plain eye. We use state-of-the-art ultrasound imaging to observe the baby’s features, while you get to catch your baby’s first stretch or curl. Knowing what happens during the scan makes the process feel a little less mysterious and a lot more reassuring. The Procedure Involved The procedure is usually done with an abdominal ultrasound, unless your doctor suggests a transvaginal scan for better visuals. You’ll lie back in a calm setting while we gently glide the probe over your bump to capture detailed images. No pain involved-it usually takes 20 to 30 minutes. This scan captures thickness behind the baby’s neck and their nasal bone, done with precision and sensitivity. Preparing for the NT Scan We suggest arriving with a full bladder to get clearer images during the scan. Emotionally, it helps to have your partner or loved one by your side – we welcome their presence during the visit. Our team guides you gently through every step, and we’re always ready to answer your questions with clarity and kindness. NT Scan Measurements and Their Relevance The numbers from an NT scan might seem puzzling at first, but they hold deeper meaning that our experts walk you through thoroughly. They are your baby’s earliest clues-signals that hint toward their health and development. Key Measurements Explained The NT measurement checks the fluid buildup under the skin behind the baby’s neck. A reading under 3.5 mm is usually considered normal at 12 weeks, though exact values depend on gestational age. We also check for nasal bone visibility – its absence could suggest a possible chromosomal issue. Elevated measurements don’t confirm problems, but they help us decide whether additional tests are needed. Combined Screening Approach We combine NT scan results with a blood test that checks hormone levels like PAPP-A and HCG. This approach increases accuracy and gives a better picture than relying on the scan alone. Our integrated test method helps us calculate risk for conditions like Trisomy 21 and provides peace of mind or early referral for care. Understanding the Results Opening your NT scan report can stir up many emotions-it helps to know what the values actually mean. Our team at Eva Womancare Clinic explains every detail so you don’t have to face that paper alone. What the Readings Indicate A typical NT reading varies with gestational age, but higher values may signal chromosomal risks like Down syndrome, Edwards, or Patau syndromes. It is only a screening tool, not a diagnosis-and serves to guide what comes next. Even if your results seem out of range, many babies develop normally, which is why follow-up is key. Next Steps After the Scan If your results suggest a higher risk, we may suggest further tests like CVS or amniocentesis for confirmation. Genetic counselling becomes important at this stage to help you make confident and informed decisions. We take the time to discuss every step based on your specific situation, ensuring you never feel rushed. Risks, Accuracy & Limitations The NT scan is safe, but understanding its strengths and blind spots helps set the right expectations. While it gives a valuable head-start into prenatal care, it doesn’t paint the whole picture on its own. Accuracy and Limitations This scan is a screening-not a diagnostic-test, which means it estimates risk, not certainty. False positives can happen, especially without the combined blood test. That’s why we always recommend additional tests if results appear unusual; it’s about making clearer decisions early. Potential Risks and Safety There’s zero physical risk to you or the baby as this scan uses standard ultrasound waves. Emotional concern is natural, which is why our compassionate approach focuses on creating a calming environment. Knowing
Burning Sensation in Urine During Pregnancy
Has that sudden burning feeling while peeing caught you off guard and left you worried and uncomfortable? Pain. Agitation. Stress. Three things every expecting mother wants to avoid-but this one symptom ticks all the boxes. Frequent bathroom runs are normal in pregnancy, but when it burns, it might signal something more than just hormones. It could be a urinary tract infection or bladder irritation-things that need the right care and attention. At Eva WomanCare clinic, we support expecting mothers through each stage-including moments like this. Our specialists combine expert diagnosis with compassionate care that understands what your body needs. Common Causes of Burning Sensation in Urine During Pregnancy Hormonal and physiological changes During pregnancy, the body undergoes constant adjustments. Hormones like progesterone relax bladder muscles, causing slow urine flow. This makes it easier for bacteria to grow. Pressure from the expanding uterus also reduces the bladder’s space to empty fully, which might lead to irritation and that sharp burning feeling. Development of urinary tract infections (UTIs) Trapped urine becomes the perfect spot for bacteria. This is why UTIs are common, especially when bacteria enter the urinary system and multiply. In some cases, you may not feel it at first, but it can turn into a painful infection if untreated. Irritation due to genital or vaginal changes Increased discharge and genital sensitivity can irritate the vaginal area. Friction, hormonal fluid shifts, and pH changes might cause itching or a mild burning feel during peeing, even without infection. Non-infectious urinary inflammation Sometimes, the bladder reacts without bacteria being present. This can be because of sensitivity to hygiene products, dehydration, or temporary inflammation. The result feels very similar to an infection but with no underlying bacteria. Recognising Symptoms and Urine-Related Changes Symptomatic UTI signs to watch for Need to pee often and urgently? If it burns or stings when you do, watch out. Pain when passing urine, along with cloudy or strange-smelling urine, can hint at an infection needing immediate attention. Changes in urine appearance and smell You might notice your urine looking darker than usual or giving off a stronger smell. These changes could be caused by hormonal shifts or might be one of the early pregnancy clues many women overlook. Other discomforts indicating infection If you feel a dull ache while emptying your bladder or a dragging sensation near your pelvis, these may accompany a growing UTI. Pain in the lower belly needs checking, especially during pregnancy. Early pregnancy urine signs Some women report subtle signs early on-like urine having a different odour or pattern. These alone aren’t proof of pregnancy but can be part of a bigger picture when combined with other symptoms. Infection-Related Pain and Associated Risks Risks of untreated infections Ignoring urine pain can lead to kidney infections. That’s when things heat up with fever, chills, and even hospital stays. It could also affect the baby’s weight or cause early delivery. Third-trimester bladder discomfort As pregnancy progresses, the uterus presses harder on the bladder. This slows urine flow, raises infection chances, and causes sharp urethral pain. Repeated pressure may heighten discomfort. Pain escalation hints serious concerns If pain changes from annoying to unbearable or comes with cramps or spasms, it could suggest the infection is spreading. It’s important to get these checked before complications arise. Possible impact on fetal well-being Unchecked infections may indirectly affect the baby’s environment. Infections during late pregnancy can increase risk during delivery or contribute to foetal distress. Early diagnosis helps keep things safe. Diagnosis and Differentiation from Pregnancy Symptoms Distinguishing UTI vs normal pregnancy discomfort Some symptoms blur lines-both pregnancy and UTIs bring tiredness, frequent urination, and pressure. But burning or persistent pain, especially during urination, points more towards infection. Diagnostic tests and urine analysis Your doctor may ask for a midstream urine sample. This simple test checks for infection indicators like white blood cells or bacterial presence. Results guide further treatment. When to report symptoms to your doctor Any new or worsening discomfort during urination shouldn’t be ignored. If the smell or colour of urine changes or you burn while peeing, report it during your next check-up. Monitoring recurring or persistent infection At Eva WomanCare Clinic, we keep a close watch during pregnancy check-ups. Recurring symptoms are flagged early, and we use screening to spot hidden infections early in the timeline. Treatment Options and Home Remedies Safe medications prescribed during pregnancy Your doctor might select antibiotics classed safe in pregnancy. The dosage depends on the stage and your personal history. It’s key to complete your course even if you feel better. Natural and home strategies Plenty of water helps flush bacteria out. Cranberry supplements and natural vitamin C sources give mild support. Warm compresses offer some ease and can reduce bladder cramps. Managing recurring infections Good hygiene and frequent changing of undergarments go a long way. We usually counsel on daily hygiene, hydration habits, or addressing any contributing conditions causing recurrences. Options during early pregnancy Treating UTIs early keeps risks lower. In early months, care is taken with antibiotics. Keeping infections away here helps prevent complications later in pregnancy. Prevention Tips and Everyday Care Daily hygiene practices We always advise from front to back wiping. Cleaning up before and after intercourse using gentle cleansers reduces bacterial travel to the urinary tract. Clothing and toilet habits Treating UTIs early keeps risks lower. In early months, care is taken with antibiotics. Keeping infections away here helps prevent complications later in pregnancy. Fluid intake and lifestyle modifications Drink enough water to keep your urine pale yellow. Set reminders if needed-hydration isn’t just comforting, it keeps bacteria away by flushing the tract regularly. Emptying bladder fully Leaning slightly forward while sitting on the toilet can help you drain the bladder better. Try not to “hold it in” too long during the day. When to Seek Medical Help? Late trimester warning signs If urination pain worsens as your due date nears, pay attention. Spotting or contractions along with burning may mean more than just a UTI.
Symptoms of Anemia in Pregnancy
Growing a baby is beautiful, but fatigue that lingers like a fog isn’t just part of the package-it’s a red flag. Many women brush it off, but this quiet weariness can snowball into something that affects both mother and baby. Pale skin, short breaths, dizzy spells-these seem harmless, until they steal your peace day after day. During pregnancy, blood volume rises, and without enough iron, your body struggles to keep up. If you’re an expecting mother trying to juggle work, home, and self-care – Eva WomanCare Clinic is here for you. We guide you with clarity, offering personalised care that brings both answers and support. Understanding Anemia During Pregnancy Definition and diagnostic thresholds Anemia during pregnancy isn’t just about feeling tired-it’s about low hemoglobin levels that strain both mother and baby. In the first trimester, hemoglobin should stay above 11 g/dL; by the third, anything below 10.5 g/dL raises concern. Severe cases drop below 7 g/dL, indicating risks that need quick care. At Eva WomanCare, we detect early warning signs through our first-trimester checkups so mothers feel safe and supported from day one. Iron and nutrient role in pregnancy Your baby thrives on oxygen, and iron helps transport it through your blood-missing that, both of you miss out. Iron boosts red blood cell creation, while folic acid prevents spinal issues and vitamin B12 supports brain development. At our clinic in Navi Mumbai, we guide mothers on personalized vitamin and iron supplementation plans to stay on track. That’s one less worry while you prepare to welcome your little one. Who is at risk? Skipping meals, back-to-back pregnancies, and untreated stomach infections quietly build the perfect storm for anemia. Women with poor dietary intake or chronic illnesses like malaria or dengue often fall deeper into deficiency without realising it. If you have a history of short pregnancy gaps or parasitic infections, talk to us early. Our expert care under Dr Grishma helps you manage such risks confidently, efficiently and professionally. Symptoms of Anemia in Pregnancy Mild to moderate symptoms Fatigue that doesn’t go away, lightheaded mornings, and pale lips-these aren’t just pregnancy quirks. They often signal low iron levels that need attention. If you’re feeling out of breath climbing stairs or find yourself napping midday, it might be your body’s way of waving a red flag. Through experience and early screenings, Eva WomanCare identifies these signs before they spiral. Severe or emergency symptoms Struggling to breathe while resting? Heart racing by just walking? It’s time to act. Fainting spells, chest pain, and struggling to stay alert can be indications of dangerously low iron levels. At Eva WomanCare, we manage these complications under our high-risk care services before it endangers your health or your baby’s. Relief starts the moment you’re heard and helped. Types of Anemia Affecting Pregnant Women Iron Deficiency Anemia This isn’t rare-it affects most expecting mothers and usually comes from low intake or poor iron absorption. It quietly chips away at energy levels and fetal growth if left untreated. Our nutrition plans help you find safe, iron-rich meals suited to your lifestyle. With Navi Mumbai’s top-rated gynaecologist by your side, you’re supported at every step. Folate and Vitamin B12 Deficiency B12 and folate keep the baby’s nervous system healthy, especially in vegetarians who may unintentionally miss out. Deficiency here may lead to birth defects or delayed development. At Eva WomanCare, we offer tests and detailed diet counselling so even plant-based mothers get what their body needs. We remove the guesswork so your growing baby gets the best support. Diagnosis and Monitoring Diagnostic tests and lab values A simple blood test uncovers more than you think. We check hemoglobin, red cell size, and ferritin levels to assess your iron stores. Peripheral smears give detailed insights to help us understand the type and severity. All of this is done through carefully guided diagnostics under Dr Grishma’s expert eye. Monitoring through pregnancy Each trimester carries different challenges, and anemia often worsens in the third. If unmonitored, it may go from mild to severe while staying silent. We recommend close tracking in later weeks through iron level checks and symptom screening. At Eva WomanCare, we tailor these assessments to individual needs. Effects on Mother and Baby Maternal health complications Tiredness is just the beginning-anemia may lead to infections, excessive blood loss after delivery, or even require a transfusion. When iron runs low, healing slows and energy disappears. With over 25 years of experience, our maternity team ensures every such risk gets managed before it becomes severe. You focus on bonding, we handle the care. Fetal development concerns Babies need iron too-for growth, weight gain, and timely delivery. Sustained deficiency may cause low birth weight or premature birth. We use ultrasound and 3rd-trimester scans to check baby’s growth and catch delays. You stay informed through every step with us. Treatment and Supplementation Standard medical treatments Anemia doesn’t wait, and neither should treatment. We begin with iron, folic acid and vitamin B12 supplements in simple, safe doses suited to your needs. Timing and duration are adjusted monthly based on how your body responds. Our continuity in care makes managing prenatal anemia less stressful. Tips for supplement intake Take iron on an empty stomach or with a slice of lemon. Avoid high fibre or calcium right after. Side effects like nausea or black stools are common-our team offers solutions to ease absorption without discomfort. You focus on feeling better, we refine what works best for your body. Nutrition and Lifestyle Management Iron-rich foods From palak paneer to mutton curry, traditional meals carry hidden iron treasures. We guide mothers through culturally relevant food plans that blend taste with nutrition. Our plans suit both vegetarian and non-vegetarian diets. Your plate becomes your strength without overcomplicating daily cooking. Enhancing absorption and avoiding inhibitors Fresh lemon juice or fermented rice boosts iron digestion naturally. But tea, milk, and excess fibre can block absorption when taken close to
Mother Baby Bonding Programs

That first touch, that first gaze-so much is said before a single word is spoken. But when stress, fatigue, and uncertainty show up uninvited, that magical connection can sometimes stumble at the start. Between sleepless nights, feeding struggles and emotional rollercoasters, many mothers feel unsure if they’re “doing it right.” Feeling unseen or unsupported shouldn’t be the norm-yet for so many, it is. At Eva WomanCare Clinic, we guide new mothers like you with gentle hands and wise hearts. Our bonding programs nurture more than just your baby-they help centre you too. Understanding Mother Baby Bonding Programs Those early moments after childbirth aren’t just emotional-they lay the foundation for a lifelong connection. At Eva WomanCare, we view mother baby bonding programs as crucial touchpoints during the early postnatal phase. These programs strengthen physical closeness and emotional warmth between mother and child, while offering structured emotional and developmental support. Our experienced team, based in Vashi, Navi Mumbai, uses both scientific insight and traditional care, helping every mother-baby pair build trust, affection, and connection day by day. Purpose and Overview of Mother Baby Bonding Programs Every newborn seeks comfort through touch, smell, and voice long before recognising words. Our programs focus on building this infant attachment by encouraging emotional responsiveness and tuning into your baby’s cues. From understanding soft whimpers during a diaper change to smiling back at baby’s first giggle, we guide mothers toward nurturing deeper maternal-child attachment using gentle, everyday infant communication techniques. With guidance from our multidisciplinary team, responses become more natural, and moments more connected. Types of Bonding Programs Available No two mothers are the same-so bonding shouldn’t follow a one-size model. We offer multiple paths to help suit your comfort and lifestyle. Bonding begins with skin-to-skin sessions right after birth at our clinic, followed by private mother-baby activities like yoga and baby massage. For ongoing connection, community circles and online workshops offer guidance, comfort, and camaraderie. Each program complements your emotional rhythm while promoting shared calm between you and your baby. Key Components of Effective Bonding Programs Real connection grows in simple joys-those shared smiles, gentle cuddles, and playful nudges. At Eva WomanCare, each bonding session brings mother-infant interaction to life through thought-out activities and shared experiences that add emotional depth to these tender moments. With 25+ years of holistic maternal care, every technique offered is grounded in what truly matters-present, loving parenting made real through touch, communication, and caring presence. Activities Encouraging Connection Touch builds trust faster than words ever could. That’s why our sessions emphasise daily baby massages, which not only soothe but promote neural development. For some, shared bath time becomes an emotional anchor-with calming splashes turning into giggles and cuddles. Through lullabies, eye contact, and repeating the baby’s name softly, everyday bonding exercises evolve into moments your child feels safe, seen, and cherished. Communication and Emotional Reciprocity Your baby may not speak, but their small gestures say so much. We help parents read those signals and respond with warmth and understanding. Describing surroundings in a calm voice or naming emotions on your own face helps babies learn how to express theirs. These exchanges-mutual gaze, mirroring sounds, responsive touches-are more than sweet moments. They’re foundational building blocks of security and empathy. Touch, Comfort, and Presence The body remembers touch long after memory fades. Within our programs, touch plays a central role-be it skin-to-skin cuddles right after birth, soft cradles during feeding, or baby-wearing throughout the day. These cosy routines are more than comforts-they build physical and emotional reassurance. Rocking, gentle patting, or lying next to your newborn at bedtime strengthens your baby’s sense of predictability and comfort for the days ahead. Benefits of Bonding on Development The effects of bonding extend far beyond the first smile. At our centre in Navi Mumbai, mothers are supported holistically because meaningful bonding deeply influences both the baby’s emotional world and growing brain. From how babies react to stress, to how they socialise, solve problems, and form affection later, our programs support development at each stage. That’s why bonding sessions aren’t add-ons-they’re essentials wrapped in love. Emotional and Social Growth Babies learn how to manage emotions through how they are held, comforted, and cared for. Our bonding programs create chances for secure infant attachment by modelling gentle responses and consistent affection. Over time, this builds a child’s sense of safety, helping them approach new people and situations with trust. It also tends to the emotional wellness of the mother, creating two emotionally resilient hearts beating together in harmony. Cognitive Development Support Babies absorb their world through rhythm, sound, and frequent interaction. Our programs encourage playful repetition-clapping, peekaboo, naming objects-that aids developmental milestones. It sparks parts of the brain responsible for memory, attention, and even early problem-solving. Through these sensory-focused activities, cognitive growth is supported naturally and joyfully. The baby not only hears you-they begin understanding and eventually responding with budding curiosity and alertness. Approaches in Indian Context In India, care begins not just in clinics but in kitchens, prayer rooms, and grandmothers’ stories. Blending these traditions with evidence-backed methods is at the heart of Eva WomanCare. Our approach fuses warm generational practices like massages and songs with data-driven care plans. Whether you’re steeped in heritage or prefer modern methods, our care honours both-the home and the clinic-as spaces for growth and bonding. Traditional and Modern Bonding Strategies Rituals like coconut oil massages or cradle songs are more than customs-they offer connections passed across generations. Many Indian homes follow 40-day postpartum support at home, rich in rest and warmth. We integrate these with structured health checkups and educational tools. Whether it’s swaddling newborns in soft cloth or explaining infant cues during breastfeeding, our team bridges tradition with insight for better child growth support. Accessing Local Services and Support In Navi Mumbai, Eva WomanCare provides seamless access to support tailored for new parents. Located near Tilak College, our clinic offers in-person bonding coaching, postnatal workshops, and live video counselling. From breastfeeding support to
Pregnancy Care Begins with Your First Doctor Check-Up

The moment you see a positive test, questions start showing up just as fast. What should I eat? When do I see a doctor? Is this feeling normal? Uncertainty can grow louder than the excitement if you let it. That’s why your first pregnancy check-up matters more than most people realise. It’s where clarity begins and where real care takes shape. Early visits help catch risks, answer questions, and build a foundation for the months ahead. This isn’t just the start of pregnancy care. It’s the start of support. When to Schedule and Why Timing Matters For most pregnancies, the first check-up should happen between 6 to 8 weeks. This is the window where your doctor can: Confirm the pregnancy Estimate your due date Screen for early risks or complications But if you have: A history of miscarriages Conditions like diabetes or thyroid imbalance Concerns about unusual symptoms …don’t wait. The earlier you’re seen, the more control you have. If you can’t make it to the clinic right away, start with a teleconsultation. It’s not just about convenience; it ensures support kicks in when it matters most. What to Expect at Your First Prenatal Check-Up The first appointment isn’t just about ticking boxes; it’s where the foundation of your pregnancy care takes shape. At Eva Woman Care Clinic, we keep this visit structured but personal, so you’re not left feeling like just another file number. Here’s what typically happens: 1. Registration and File Creation You’ll be welcomed by our front desk team and guided through a short registration process. We’ll create your personal pregnancy file, covering essentials like: Medical history Insurance details Any past or ongoing health concerns Not sure what to carry? Just bring your ID, any previous reports, and we’ll take care of the rest. 2. Health and Physical Examination A routine health check includes: Height, weight, and BMI Blood pressure and pulse A gentle pelvic exam to assess uterine changes This helps us confirm pregnancy progress and spot any red flags early, before they become problems. 3. Confirming Pregnancy and Location Depending on your timing, a transvaginal scan may be done to confirm fetal location and rule out ectopic pregnancy. We walk you through every step so you’re not just getting checked, you’re understanding what’s being checked and why it matters. Core Diagnostic Tests at the First Visit What’s happening inside matters just as much as how you feel on the outside. Your first check-up includes essential screenings to map your health profile and identify any early risks. At Eva Woman Care Clinic, the majority of tests are conducted in-house to keep your journey smooth and coordinated. Blood Tests Typically Include: Blood group and Rh factor Hemoglobin and sugar levels Thyroid function (TSH) Immunity screening for rubella HIV, Hepatitis B, and syphilis panels These results help us catch common issues like anaemia, gestational diabetes, or infections before symptoms even appear. Urine Test We’ll check for signs of infection, dehydration, or excess protein, all of which can point to early pregnancy complications. Ultrasound and Due Date Estimation An early scan gives us a clearer picture of your baby’s age, position, and whether you’re carrying multiples. We calculate your Estimated Due Date (EDD) based on this scan or your last period, whichever is more accurate. Optional Genetic Screening If needed, we may recommend first-trimester screenings like: Nuchal translucency (NT) scan Non-invasive prenatal testing (NIPT) These help assess chromosomal health, especially for women with a family history or advanced maternal age. You’re never left guessing; we explain what’s being done, what the results mean, and what your next steps should be. Doctor’s Guidance: Nutrition, Supplements & Lifestyle Care doesn’t end with tests. At your first appointment, we’ll walk through how your daily habits can support a healthy pregnancy, without overwhelming you with conflicting advice. Food: What to Focus On You don’t need to “eat for two.” You need to eat smart. We’ll guide you on: Foods rich in folate, iron, and calcium What to avoid: raw meats, unpasteurised dairy, alcohol, excess caffeine Tips for managing nausea, acidity, and fatigue through meal timing You’ll leave knowing what fuels your body, not just what to avoid. Supplements: Backing Your Diet Even with a balanced diet, supplements are essential in early pregnancy. Based on your needs, we may start: Folic acid (to reduce neural tube risks) Iron (to prevent anaemia) Calcium (for bone support) We adjust for vegetarians, dietary restrictions, or existing conditions. Everything is prescribed based on your bloodwork, not guesswork. Lifestyle: What to Shift Gently We also cover simple, realistic changes: Improving sleep hygiene Staying active with short walks or light prenatal stretches Managing screen time before bed It’s less about rules, more about rhythms that make each day easier to handle. Mental Health and Emotional Check-In Pregnancy isn’t just physical; it affects your mood, sleep, and state of mind. That’s why we take mental health seriously from the very first visit. At Eva Woman Care Clinic, we ask how you’re really doing, because stress and anxiety show up early and often go unnoticed. What You Might Feel Mood swings or irritability Restlessness or poor sleep Feeling overwhelmed by small things These may feel like signs of weakness, but they’re common hormonal shifts, and you’re not alone. How We Support You Time during your check-up to talk openly No judgement, no brushing things off Recommendations for rest, breathing routines, or supportive resources if needed We don’t wait for mental health to become a problem. We check in early and often, so you feel heard, not just examined. Building Your Pregnancy Care Roadmap Pregnancy unfolds in stages, each with its own milestones and medical needs. Your first prenatal visit includes setting a plan that evolves with you, and this is how Eva Woman Care Clinic supports that journey without exaggeration. Visit Schedule by Trimester Most patients follow this basic rhythm: Weeks 0–28: Monthly check-ups Weeks 28–36: Every two weeks Weeks 36 onward: Weekly monitoring High-risk cases get additional visits or early interventions. Personalised
Best Nutrition During Pregnancy: What Should Mums Eat?

One day, it’s dry toast and lemon water. The next it’s a desperate search for pickles at 2 a.m. Pregnancy eating can feel like a rollercoaster with your body, your brain, and your taste buds all trying to take the wheel. Everyone has advice. Most of it is conflicting. You’re told to eat more, but not too much. Cut out spicy food, but don’t skip the nutrients. Drink milk, but not cold. The noise is constant, and the decisions still land on your plate. At Eva Woman Care Clinic, we understand how overwhelming pregnancy nutrition can be. The goal is not perfection. It’s a balance. And that balance begins with understanding what your body really needs, trimester by trimester, day by day. Core Nutrition Principles for Pregnancy Pregnancy is not about eating twice as much; it’s about eating smart. Your body’s nutritional needs increase, but that does not mean portion overload. It means choosing meals that give you sustained energy, essential nutrients, and digestive support. Macronutrients Matter Carbohydrates fuel your body and help stabilise mood swings. Opt for whole grains, fruits, and cooked root vegetables. Proteins are the building blocks. Dals, paneer, eggs, or lean meats support both fetal development and maternal strength. Healthy fats like nuts, seeds, and small amounts of ghee aid brain development and keep your hormones in check. Micronutrients Carry Weight Folic acid: Prevents neural tube defects. Found in spinach, oranges, and fortified grains. Iron: Supports blood volume and energy. Present in jaggery, lentils, and leafy greens. Calcium and Vitamin D: Needed for bone strength, for both mother and baby. Iodine, magnesium, and zinc: Often forgotten, but crucial for metabolism, thyroid health, and tissue repair. Timing and Consistency Regular, well-spaced meals help manage nausea, blood sugar dips, and fatigue. Skipping meals may increase discomfort or cause heartburn later in the day. Pregnancy is demanding. Nutrition is your daily fuel, not your daily stress. Trimester-Wise Nutrition Breakdown Your body changes fast during pregnancy, and so do its nutritional priorities. What works in the first trimester might not cut it later on. Here’s how to adapt your food choices as each phase unfolds. First Trimester: Build the Foundation This phase is often about surviving the nausea while still feeding the essentials. Focus on: Folate-rich foods: Oranges, spinach, rajma, and fortified cereals Light, frequent meals to manage queasiness Hydration: Coconut water, nimbu pani, and clear soups keep things moving Avoid strong smells and heavy spices. If you’re struggling to eat, even dry toast and poha can help hold you steady. Second Trimester: Support Growth and Strength As energy returns, appetite often improves; this is when the baby’s bones, muscles, and brain begin serious development. Prioritise: Calcium: Found in dairy, sesame seeds, and green vegetables Iron: Prevents fatigue; include lentils, beets, and jaggery Omega-3 fats: Flaxseeds, walnuts, or low-mercury fish Protein variety: Mix dals, sprouts, and homemade paneer This is the time to build strength, not just manage symptoms. Third Trimester: Prepare for Delivery Your baby’s weight increases rapidly now, and digestion may slow down. Shift to: Smaller, protein-rich meals: Khichdi, daal soup, and multigrain rotis Vitamin K sources: Spinach, broccoli, eggs Fibre and fluids: To ease constipation and reduce swelling Fatigue might return. That’s normal. Stick with energy-boosting snacks like bananas, sweet potatoes, or roasted nuts to stay steady through the day. Building a Simple Indian Meal Plan Eating well during pregnancy doesn’t require fancy recipes or imported ingredients. You just need the right combinations, a little prep, and foods that respect your routine. A Sample Day on the Plate Here’s what a balanced day might look like, easy to customise based on appetite and schedule. Morning Start (Before Breakfast) Soaked almonds or walnuts Warm water with lime or ajwain Breakfast Oats upma or poha with peas Idli with curd and chutney Herbal tea or milk Mid-Morning Snack Fresh fruit like guava, papaya, or apple Coconut water or buttermilk Lunch One bowl of dal Two rotis or a portion of rice Seasonal sabzi and a side of curd A few slices of salad Evening Roasted chana or foxnuts Fresh juice or herbal tea Dinner Dalia khichdi or moong dal stew Light subzi or soup One small roti or half a cup of rice Stewed fruit or a handful of raisins The idea is variety, balance, and digestibility, not stuffing in calories. Make-Ahead and Busy-Day Options Not every day allows for perfect prep. For those on the go or managing work and home: Dry fruit laddoos: Easy to carry, rich in iron and protein Sprout salad: Prepped in advance, tossed fresh Roasted peanuts or makhana: Great for tea-time hunger Boiled eggs or paneer cubes: Fast, protein-packed snacks Herbal tea bags: Calming, hydrating, and caffeine-free Eva Woman Care Clinic often shares meal ideas that work across different pregnancy stages and dietary preferences, especially for vegetarian mums looking to hit key nutrient marks. Foods to Include and Avoid Pregnancy is not the time for trendy diets or crash restrictions. Your body needs fuel that works hard and digests easily. Some foods strengthen you. Others? They just complicate the process. What to Include: Everyday Nutritional Powerhouses These foods tick multiple boxes: nutrient density, digestibility, and pregnancy-safe profiles. Whole grains: Brown rice, bajra, and jowar offer energy without sugar spikes Dals and legumes: Moong, masoor, and chana are rich in iron, protein, and fibre Dairy: Toned milk, curd, paneer for calcium and gut support Nuts and seeds: Almonds, walnuts, and flaxseeds are healthy fats and brain boosters Leafy greens: Spinach, methi, and curry leaves offer folate, iron, and vitamin K Fruits: Guava, papaya (ripe), banana, berries aid in digestion, boost immunity, and hydration Low-mercury fish (if non-vegetarian): Sardines, rohu, salmon, rich in omega-3 and protein Keep the focus on local and seasonal. They’re easier on your body and richer in bioavailable nutrients. What to Avoid: High Risk and Low Value Some foods offer more risk than reward, especially when digestion, immunity, and the baby’s development are on the line. High-mercury fish: King mackerel,
Can Surya Namaskar Help with PCOS? A Doctor’s Perspective

PCOS doesn’t show up quietly. It disrupts cycles, energy, skin, mood and confidence. Many women wake up to a body that feels unpredictable. Bloating, cravings, fatigue, it’s a rotating script with no warning. That’s what leads so many to look beyond prescriptions. Yoga often enters the conversation. But can Surya Namaskar actually support hormone balance? This isn’t about spiritual fluff. It’s about function. And how one sequence of movement might give your system a chance to steady itself. What Happens in the Body with PCOS PCOS begins with hormonal misfires, usually too many androgens. Ovulation takes a hit. Insulin builds resistance. Fat settles around the belly. Cycles stretch longer. Anxiety creeps in. Sleep gets worse. The body stops working in rhythm. And when hormones lose rhythm, everything does. Medication helps. But for most women, the real shift comes with daily habits. And that’s where movement (done right) can begin to matter. Surya Namaskar: What It Is and Why It Stands Out Surya Namaskar is a sequence of 12 yoga postures. Each one flows into the next, paired with breath. It’s low-impact, full-body, and designed to wake up the spine, core, lungs, and major hormone-regulating organs. It’s not just stretching. It activates the thyroid, pancreas, and ovaries. It builds circulation. And more importantly, it calms the nervous system. Unlike random gym routines, Surya Namaskar combines stress relief with metabolic stimulation. That makes it highly relevant for PCOS. At Eva Woman Care Clinic, we’ve seen women pair it with treatment to support better cycles, reduce bloating, and stabilise mood. Not a cure. But a powerful addition to the care plan. Can Surya Namaskar Influence Hormonal Health? Let’s cut through the hype; Surya Namaskar won’t “fix” hormones overnight. But done consistently, it can support how your endocrine system performs. Here’s what matters: PCOS often comes with insulin resistance, elevated cortisol, and disrupted ovulation. These are deeply linked to stress, inflammation, and circulation. Surya Namaskar activates key hormonal sites (thyroid, adrenal glands, pancreas) through targeted movement and breath. It improves blood flow, calms the nervous system, and helps regulate insulin response. Women who include Surya Namaskar in their weekly routine often report: More regular periods Lower cravings and fatigue Improved mood stability It’s not a solo strategy. But in tandem with treatment, it helps the body regain some of its lost rhythm. Targeted Benefits for PCOS Symptoms When done consistently and under guidance, Surya Namaskar offers direct benefits for some of the most stubborn PCOS symptoms: 1. Menstrual Irregularity The combination of movement and breath helps reset the body’s internal clock. With improved blood flow to the ovaries and reduced inflammation, cycles can become more predictable. 2. Hormone-Linked Weight Gain Surya Namaskar engages the full body. It increases calorie burn, strengthens the core, and helps counter insulin resistance, one of the key drivers of PCOS-related fat retention. 3. Stress and Mood Swings By calming the sympathetic nervous system, it reduces cortisol spikes. That, in turn, makes it easier for the body to manage appetite hormones and emotional reactivity. 4. Fatigue and Brain Fog The breath-focused movement boosts oxygenation and circulation. Patients often report higher energy and better focus, even after just a few weeks of practice. None of this is magic. It’s physiology. When your body moves well, it starts responding better. And that’s the point. Who Should Approach with Caution While Surya Namaskar is safe for most, it isn’t universal. There are situations where the sequence should be adapted or paused entirely. If you’re dealing with: Severe obesity or joint pain Lower back issues or spinal injuries Early pregnancy or IVF treatment cycles …it’s important to consult your doctor first. Not all PCOS cases look the same. Some women need modified postures. Others may benefit more from restorative yoga or breathwork initially. At this stage, personalisation matters more than repetition. The wrong kind of strain can set you back, especially if hormone therapy or fertility support is already in motion. How to Start: Doctor-Approved Guidelines If you’re cleared to begin, keep it simple. No 60-minute sessions or Insta-perfect poses. Start where your body is. Here’s a basic approach: Begin with 5 rounds, 3–5 days a week Practice on an empty stomach, ideally in the morning Focus on breath more than speed, inhale on upward moves, exhale on downward ones Rest between rounds if needed When fatigue hits or symptoms flare, drop the pace, not the habit. Gentle practice still supports hormonal health. At Eva Woman Care Clinic, we often suggest Surya Namaskar in the personalised care plan, blending movement, medication, and nutrition to get better long-term outcomes. Consistency beats intensity. The goal isn’t a sweat session; it’s to create an internal rhythm. Supporting Care Beyond the Mat Surya Namaskar can move a lot, but it works best when paired with daily habits that lower inflammation and support hormone health. Here’s what we recommend building around your practice: 1. Nutrition that backs your cycle Stick to whole foods like vegetables, pulses, lean protein, and low-GI fruits. Cut back on refined sugar, processed snacks, and excessive dairy. Foods like flaxseed, spinach, and pumpkin seeds support insulin balance and reduce bloating. 2. Daily movement variety On days you skip Surya Namaskar, go for a walk or stretch. Light strength training twice a week helps balance hormones too. It doesn’t have to be hard, just regular. 3. Sleep and screen control Protect your rest. Go to bed around the same time daily. Avoid screens for an hour before sleep. Even 10 minutes of quiet breathwork can reset your nervous system. This isn’t about rigid rules. It’s about creating a body that’s easier to live in. Finding Rhythm Again Starts With One Step When you live with PCOS, it’s easy to feel like your body’s working against you. The symptoms are scattered, the cycles inconsistent, and the solutions often overwhelming. But movement done right can bring some order back. Surya Namaskar offers more than just flexibility or calm. It creates structure. It supports systems that often go
Second Pregnancy After 35: What’s Different This Time

The first time felt like stepping into unknown water – exciting, confusing, a little terrifying. Now, you’re a little older, a bit wiser, but still faced with new worries. Feeling unsure about fertility, energy levels, or baby safety is common – but so is finding calm when guided right. The truth? This time, your body might feel slower. You may need a longer time for recovery. Perhaps you need doctor visits more frequently. But with the right care, managing things like gestational diabetes, genetic screenings, or birth planning becomes smoother and far less overwhelming. At EVA Woman Care Clinic, we support women through every stage – with updated advice, emotional care, and expert-led plans fit for today’s needs. If you’re 35+ and planning baby number two, we’re here to walk beside you. Understanding the Differences in a Second Pregnancy After 35 Being pregnant again after 35 can feel like returning to a book with new pages added. You know some of the story, yet the plot takes a few surprising turns. With more life behind you and responsibilities at hand, this pregnancy brings different physical shifts and emotional moments that can feel more intense than the first. At Eva Woman Care Clinic, we make sure you’re supported through every moment – mentally, emotionally, and medically. Physical and Emotional Contrast with the First Pregnancy The second time around, symptoms may turn up sooner and feel stronger. Fatigue settles in quicker, and back pain might show up with more gusto. Your belly could pop out earlier, and baby kicks start a tad sooner too. Emotionally, juggling your firstborn’s needs while managing your own body’s demands can lead to impatience or guilt. Coping means accepting this pregnancy isn’t the first – and that’s okay. We help mums manage stress better through guided support, rest planning, and practical advice tailored to their stage. Hormonal and Biological Shifts Hormones like estrogen and progesterone continue to rise, but with age, their effect feels different. Your skin may feel drier, appetite shifts dramatically, and hair thickness might take a dip. There’s also more fluctuation in mood, sometimes making you feel unlike yourself. Our team focuses on stabilising this with safe monitoring and check-ups. At Eva Woman Care Clinic, we treat not just the belly but the whole woman – head to toe, hormone to heartbeat. Fertility and Conception Over 35 Trying for the second baby after 35 isn’t as spontaneous as before. Conception may take longer, and planning matters more. Whether this baby was long hoped for or a happy surprise, understanding the body’s readiness is the first step. With Dr Grishma’s 25+ years of insight, we guide women every day through age-linked fertility paths with compassion and expertise. Understanding Decline in Fertility As women cross 35, egg quality and ovarian reserve naturally decline. If your partner is also over 40, his fertility may shift too. Irregular cycles or delays in conception could signal it’s time to consult a specialist. At Eva Woman Care Clinic, we provide fertility support like IUI, IVF, and ICSI when needed, monitoring cycles carefully and advising on best routes forward. Early awareness makes all the difference. Planning the Right Gap Between Pregnancies Spacing between the first and second pregnancy is more than a number. Too short a gap can impact your body’s healing; too long may affect fertility. Experts suggest 18 to 24 months between births for balanced recovery. But emotional readiness, your child’s age, and support systems also matter. We help parents think through all aspects – from your energy to your toddler’s emotional needs – before deciding. Increased Health Considerations and Risks After 35, second pregnancies require gentler attention. Slight changes in blood pressure or sugar levels can become serious if left unchecked. But with frequent monitoring and timely support, we help you avoid complications and carry with calm confidence. Each mum deserves peace of mind – and we prioritise that. Common Pregnancy Complications After 35 Some women experience gestational hypertension or signs of preeclampsia like headaches, swelling, or blurred vision. These need close tracking. High blood pressure raises risk to both mother and baby, so regular checks are critical. Our clinic designs personalised care plans that include early spotting of such risks and advice that’s respectful yet practical. You stay informed – not alarmed. Special Medical Precautions and Screenings At Eva Woman Care Clinic, we recommend health screenings early and consistently. After 35, non-invasive prenatal testing becomes more relevant to check for chromosomal changes like Down Syndrome. Ultrasounds, blood checks, and genetic consultations are part of our standard process. Leveraging our in-house diagnostic expertise ensures nothing gets missed. You focus on rest; we focus on every detail. Health and Wellness Tips for Older Second-Time Mothers Energy feels more precious and the need for self-care louder this time. Nutrition, activity, and rest pull more weight in older pregnancies. Our focus at Eva Woman Care Clinic is making wellness realistic, not overwhelming – one steady habit at a time. Adopting a Pregnancy-Safe Lifestyle Low-impact workouts like walking or prenatal yoga help reduce swelling and boost circulation. Short routines keep energy up without exhaustion. We steer mums towards activities that feel joyful, not punishing. A positive outlook often starts by simply moving more gently and surrounding yourself with encouragement. At our clinic, we believe how you feel matters as much as what the scale says. Nutrition, Supplements, and Hydration Folic acid, iron, DHA, and calcium become even more important now. Simple Indian foods like ragi, lentils, and leafy vegetables help meet most needs. Too much spice or outside food may upset digestion. Fluids, especially in humid cities like Navi Mumbai, need to be increased. We guide mothers on daily intake, right snacks, and prenatal vitamins based on their lab results and overall body needs. Preparing the Family for a New Arrival Your growing belly isn’t the only thing changing – your family rhythm does too. Preparing your partner and first child emotionally goes a long way in easing everyone’s adjustment. We
How to Take Care in the First Month of Pregnancy

Pregnancy is an exciting journey, and the first month marks the beginning of a significant change in your body. Whether you’re a first-time mom or have experienced pregnancy before, it’s essential to take extra care during this time to ensure both your health and your baby’s development. In this blog, we will discuss how to take care during the first month of pregnancy, providing essential tips to help you have a healthy and smooth start to your pregnancy journey. Your First Month of Pregnancy: What to Expect The first month of pregnancy is crucial for the development of your baby. During this time, the fertilized egg implants into the uterus, and the placenta begins to form. While many women may not feel any significant changes right away, it’s still a vital period for ensuring a healthy pregnancy. You may start noticing subtle symptoms like morning sickness, fatigue, or frequent urination, but others may not show up until later in the pregnancy. Regardless, taking proper care during this early stage can contribute to a positive experience and ensure a healthy start for your baby. Tips for Taking Care During the First Month of Pregnancy 1. Schedule Your First Prenatal Appointment One of the first things you should do once you suspect you’re pregnant is to schedule an appointment with your obstetrician or gynecologist. During this visit, they will confirm the pregnancy and give you a comprehensive checkup. Early prenatal care is essential to monitor your health and the development of your baby. Key points to discuss with your doctor during your first visit: Medical history Prenatal vitamins, including folic acid Blood work and urine tests Screening for any potential complications 2. Start Taking Prenatal Vitamins Folic acid is one of the most critical nutrients during the early stages of pregnancy. It helps prevent birth defects, especially those that affect the brain and spine. Most doctors recommend starting prenatal vitamins as soon as you confirm your pregnancy. These vitamins typically contain folic acid, iron, calcium, and other nutrients important for fetal development. Why are prenatal vitamins important? Prevent neural tube defects (e.g., spina bifida) Support a healthy immune system Promote strong bones for both mother and baby 3. Stay Hydrated Drinking plenty of water is vital during pregnancy to support both your body’s increased blood volume and your baby’s growth. Dehydration can lead to complications like fatigue, headaches, and constipation. Aim for at least 8-10 glasses of water daily. Additional hydration tips: Avoid sugary drinks and caffeine Drink water regularly throughout the day Keep a water bottle with you at all times to remind yourself to hydrate 4. Eat a Balanced Diet A nutritious and balanced diet is essential in the first month of pregnancy. Focus on eating foods rich in vitamins, minerals, and proteins. Include plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats in your daily meals. Key foods to include in your diet: Leafy greens for folate Lean meats for iron and protein Whole grains for fiber and energy Dairy products for calcium 5. Avoid Harmful Substances The first month is a critical period for your baby’s development, so it’s essential to avoid anything that could potentially harm your pregnancy. Here are some things to avoid: Alcohol: It can affect the development of the baby and increase the risk of birth defects. Caffeine: Limit your caffeine intake to less than 200 mg per day. Smoking: Smoking can harm the placenta, leading to complications. Certain medications: Always check with your doctor before taking any prescription or over-the-counter medications. 6. Get Plenty of Rest Fatigue is common during the first month of pregnancy. Your body is going through many changes, and you may find yourself feeling more tired than usual. It’s important to get plenty of rest to give your body the energy it needs to support your pregnancy. Sleep Tips: Try to go to bed at the same time each night. Take naps during the day if you feel overly tired. Keep a sleep-friendly environment (dark, cool, and quiet). 7. Exercise Lightly While intense workouts should be avoided during the first month, light exercise can be beneficial for both you and your baby. Simple activities like walking or prenatal yoga can help keep your body strong and flexible. Always check with your doctor before starting any new exercise routine during pregnancy. Benefits of light exercise during pregnancy: Reduces stress Improves circulation Helps maintain a healthy weight 8. Monitor Your Symptoms During the first month of pregnancy, you may experience a variety of symptoms such as nausea, breast tenderness, frequent urination, and mood swings. While these symptoms are normal, it’s important to monitor them and report anything unusual to your doctor. Severe cramping, bleeding, or severe nausea could indicate potential complications. Conclusion The first month of pregnancy is an exciting yet delicate time, so taking good care of your health is essential. From scheduling your first prenatal appointment and taking prenatal vitamins to eating well, staying hydrated, and avoiding harmful substances, these steps will help set you on the right path for a healthy pregnancy. Taking proper care during this time also builds the foundation for your baby’s growth and development. By following these tips and staying in close contact with your healthcare provider, you’ll be setting yourself up for a smooth and healthy pregnancy journey. Frequently Asked Questions (FAQs) What symptoms should I expect in the first month of pregnancy? Common symptoms in the first month include morning sickness, fatigue, bloating, breast tenderness, and frequent urination. However, every pregnancy is different, so it’s important to pay attention to your body and consult with your doctor if you have concerns. How can I avoid miscarriage during the first month of pregnancy? While there is no way to guarantee a miscarriage-free pregnancy, there are steps you can take to increase the likelihood of a healthy pregnancy, including avoiding harmful substances, taking prenatal vitamins, eating a balanced diet, and attending regular prenatal checkups. Can I exercise in the first month
